Artificial intelligence in HealthCare

Artificial intelligence in healthcare is the use of complex algorithms and software, or in other words, artificial intelligence (AI), to emulate human cognition in the analysis, interpretation, and comprehension of complicated medical and healthcare data.
AI algorithms behave differently from humans in two ways: (1) algorithms are literal: if you set a goal, the algorithm can't adjust itself and only understand what it has been told explicitly, (2) and some deep learning algorithms are black boxes; algorithms can predict with extreme precision, but not the cause or the why.
The primary aim of health-related AI applications is to analyze relationships between prevention or treatment techniques and patient outcomes.[2] AI programs have been developed and applied to practices such as diagnosis processes, treatment protocol development, drug development, personalized medicine, and patient monitoring and care.

Implementation
The ability to interpret imaging results with radiology may aid clinicians in detecting a minute change in an image that a clinician might accidentally miss. A study at Stanford created an algorithm that could detect pneumonia at that specific site, in those patients involved,
AI to describe and evaluate the outcome of maxillo-facial surgery or the assessment of cleft palate therapy in regard to facial attractiveness or age appearance
In psychiatry, AI applications are still in a phase of proof-of-concept. Areas where the evidence is widening quickly include chatbots, conversational agents that imitate human behaviour and which have been studied for anxiety and depression.

Challenges include the fact that many applications in the field are developed and proposed by private corporations, such as the screening for suicidal ideation implemented by Facebook in 2017.[40] Such applications outside the healthcare system raise various professional, ethical and regulatory questions
There are many diseases and there also many ways that AI has been used to efficiently and accurately diagnose them
Electronic health records are crucial to the digitalization and information spread of the healthcare industry. However, logging all of this data comes with its own problems like cognitive overload and burnout for users. EHR developers are now automating much of the process and even starting to use natural language processing (NLP) tools to improve this process.
Improvements in natural language processing led to the development of algorithms to identify drug-drug interactions in medical literature.[53][54][55][56] Drug-drug interactions pose a threat to those taking multiple medications simultaneously, and the danger increases with the number of medications being taken
Improvements in natural language processing led to the development of algorithms to identify drug-drug interactions in medical literature.[53][54][55][56] Drug-drug interactions pose a threat to those taking multiple medications simultaneously, and the danger increases with the number of medications being taken.
AI needs to undergo extensive clinical validation before healthcare providers feel comfortable relying on it during regular care, Fleureau said. That means both proof-of-concept investigations from academics and real-world deployments headed by stakeholders
But there are some components of patient care where even a final-stage, fully adopted algorithm would fall short, he continued. Chief among these is the decidedly human quality of empathy.
Doctors care about the individual, the person, and so it is fair to believe that in the future one of the key roles played by doctors ... will be to be the person in the healthcare organization to have transgression rights.
There is something way more important in the relationship between a patient and a doctor. And there's a very simple reason to that: it's because there are many decisions and questions in medicine for which there is no right or wrong answer.

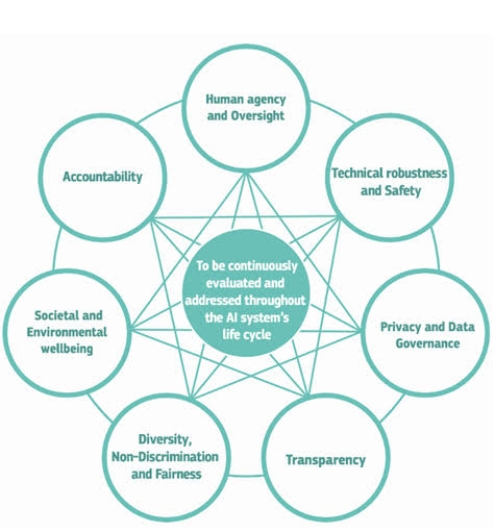
Key challenges for the translation of AI systems in healthcare include those intrinsic to the science of machine learning, logistical difficulties in implementation, and consideration of the barriers to adoption as well as of the necessary sociocultural or pathway changes. Robust peer-reviewed clinical evaluation as part of randomised controlled trials should be viewed as the gold standard for evidence generation, but conducting these in practice may not always be appropriate or feasible. Performance metrics should aim to capture real clinical applicability and be understandable to intended users. Regulation that balances the pace of innovation with the potential for harm, alongside thoughtful post-market surveillance, is required to ensure that patients are not exposed to dangerous interventions nor deprived of access to beneficial innovations. Mechanisms to enable direct comparisons of AI systems must be developed, including the use of independent, local and representative test sets. Developers of AI algorithms must be vigilant to potential dangers, including dataset shift, accidental fitting of confounders, unintended discriminatory bias, the challenges of generalisation to new populations, and the unintended negative consequences of new algorithms on health outcomes.
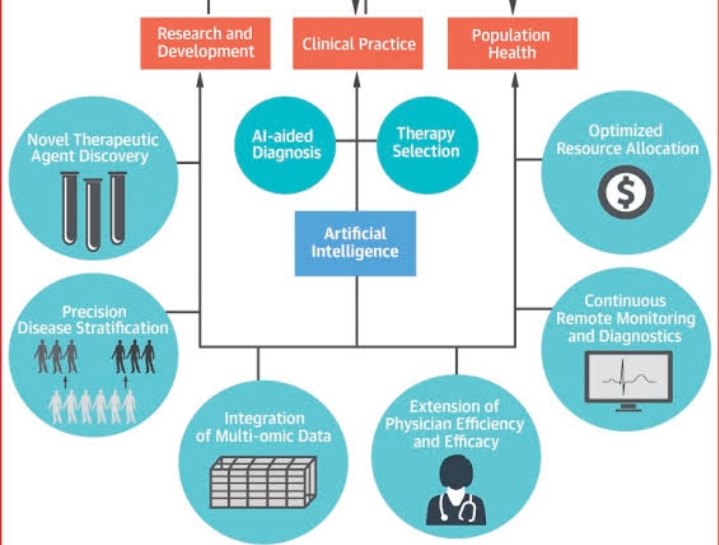
Use cases of AI Artificial intelligence simplifies the lives of patients, doctors and hospital administrators by performing tasks that are typically done by humans, but in less time and at a fraction of the cost.
PathAI is developing machine learning technology to assist pathologists in making more accurate diagnoses. The company's current goals include reducing error in cancer diagnosis and developing methods for individualized medical treatment.
Buoy Health is an AI-based symptom and cure checker that uses algorithms to diagnose and treat illness. Here's how it works: a chatbot listens to a patient’s symptoms and health concerns, then guides that patient to the correct care based on its diagnosis
Freenome uses AI in screenings, diagnostic tests and blood work to test for cancer. By deploying AI at general screenings, Freenome aims to detect cancer in its earliest stages and subsequently develop new treatments.
BERG is a clinical-stage, AI-based biotech platform that maps diseases to accelerate the discovery and development of breakthrough medicines. By combining its “Interrogative Biology” approach with traditional R&D, BERG can develop more robust product candidates that fight rare diseases.
Atomwise uses AI to tackle some of today's most serious diseases, including Ebola and multiple sclerosis. The company's neural network, AtomNet, helps predict bioactivity and identify patient characteristics for clinical trials.
In the healthcare industry, time is money. Efficiently providing a seamless patient experience allows hospitals, clinics and physicians treat more patients on a daily basis.
Olive’s AI platform is designed to automate the healthcare industry' most repetitive tasks, freeing up administrators to work on higher-level ones. The platform automates everything from eligibility checks to un-adjudicated claims and data migrations so staffers can focus on providing better patient service


